NEWSROOM
-
Professor Zhiguo Luo and Professor Xin Liu from the Fudan University Shanghai Cancer Center published an article in Cancer Research and Treatment recently, summarizing the patient cohort of Inflammatory Myofibroblastic Tumor (IMT) treated in our center in the past 15 years, providing valuable clinical case data of IMT in the Chinese population. It is also the largest data on adult IMT cases to date.
Overall, 102 IMT patients were identified in our institution from 2006 to 2021. Among them, 39 patients were aged ≥ 18 years old. Nine patients with insufficient follow-up data were excluded. Therefore 30 patients were enrolled in the present study. The age range of the 30 adult patients was 21-77 years, with a median age of 38 years. Twelve patients were men (40.0%), and 18 were women (60.0%). The most common primary lesions were those in the abdomi?nopelvic region (n=16; 53.3%), followed by the lungs (n=6, 20.0%), and retroperitoneum (n=2, 6.7%). The most common presenting symptoms were abdominopelvic discomfort (18/30, 60%), fever (6/30, 20%), cough (5/30, 16.7%), and weight loss (4/30, 13.3%). Seven had abdominal EIMS. 36.7% (11/30) had localized disease, and 63.3% (19/30) had metastatic or inoperable diseases. Liver (10%, 3/30) was the most common site of distant metastases.
Twenty-seven patients were tested for ALK expression by IHC or for gene rearrangement by FISH. The ALK posi?tivity rate was 81.5% (22/27). The consistency rate of ALK immunohistochemistry and gene rearrangement was 100%. All patients with EIMS were ALK-positive. In patients with ALK-negative and ALK-positive tumors, the median age was 50 years (range, 34 to 77 years) and 30 years (range, 21 to 74 years), respectively. NGS was per?formed in four patients, and TPM3-ALK rearrangement, RANBP2 (RAN binding protein 2)–ALK rearrangement, and IGFBP5 (insulin like growth factor binding protein 5)–ALK rearrangement were detected; one patient had no targetable genetic abnormality.
Of the 19 patients who underwent radical surgery, eight (42.1%) had recurrence and/or metastasis after surgery. The time from surgery to relapse and/or metastasis of these eight patients ranged from 4.5-26.1 months (medi?an time, 8.3 months; 95% confidence interval [CI], 7.3 to 9.4 months).
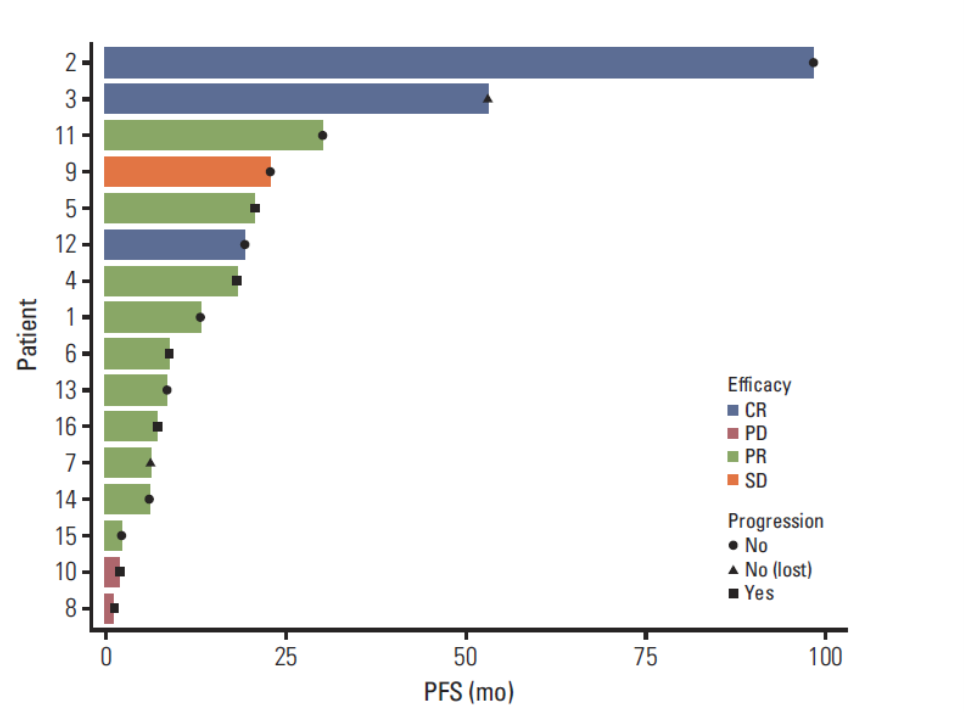
In total, 16 patients with advanced ALK-positive IMT were treated with crizotinib (an oral small-molecule inhibitor of ALK, MET, and ROS1) at a dose of 250 mg twice daily. 10 (62.5%) had PR, three (18.8%) achieved CR, one (6.3%) had SD, and two (12.5%) had PD. ORR was 81.3% (13/16), and DCR was 87.5% (14/16). At a median follow-up time (from the time of crizotinib) of 23.0 months (95% CI, 16.5 to 29.5 months), the median PFS was 20.8 months (95% CI, unreached). The 1-year PFS rate was 70.7% (58.1%-83.3%). The median OS for systemic treatment was not determined. The 2-year OS for systemic treatment rate was 78.1% (63.0%-93.2%).
Up to February 2022, the median follow-up period (from the time of diagnosis) of all 30 patients was 30.0 months (95% CI, 13.6 to 46.4), and the 1-year, 3-year, and 5-year OS rates were 96% (95% CI, 93 to 99), 85% (95% CI, 76 to 93), and 77% (95% CI, 66 to 88), respectively (Fig. 3). Four patients were diagnosed with multiple primary can?cers (MPC).
The results of this study suggest that adult IMT cases appear to be more aggressive, with a higher incidence of recurrence and metastasis. Also, ALK rearrangements are a common genetic abnormality. Crizotinib showed a high ORR and durable response in patients with advanced adult IMT. A next generation of ALK inhibitors could be used as treatment options for patients with crizotinib-resistant, ALK-positive IMT. The role of the ALK signaling pathway in adult IMT and the mechanism of drug resistance to ALK inhibitors are worthy of further study from clinical and basic aspects.
Fig. 1 shows images of a patient with uterine IMT harboring an IGFBP5-ALK rearrangement who achieved PR after crizotinib treatment. The patient had an abdomin-opelvic region and lymph node metastases when first diag?nosed. After treatment with crizotinib for > 10 months, the tumor showed PR. This patient was still receiving crizotinib treatment at the time of the analysis.
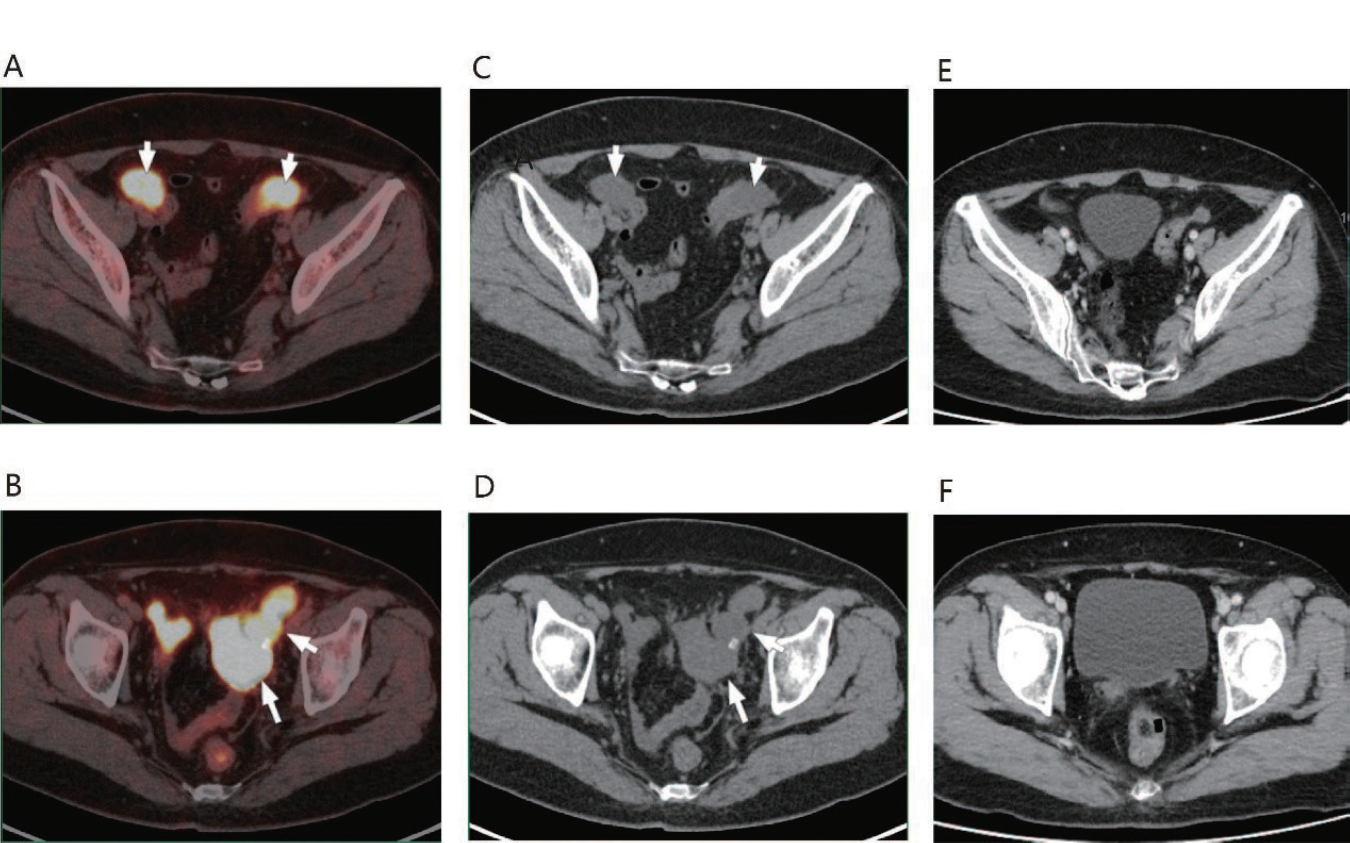
Fig. 2. Swimming plot of adult inflammatory myofibroblastic tumor patients. CR, complete response; PD, progression disease; PR, partial response; SD, stable disease.